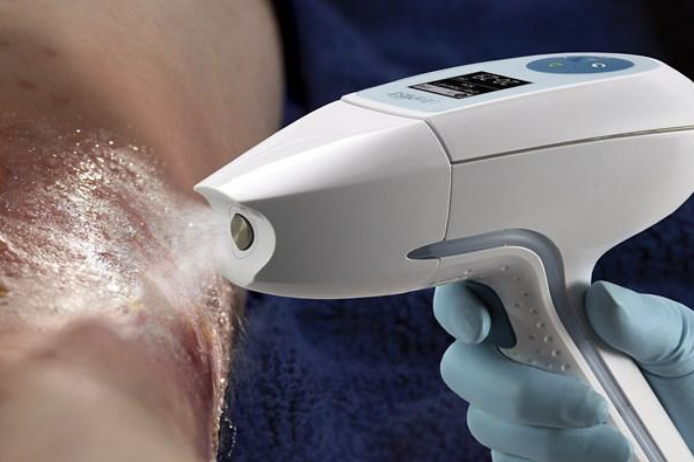
What You’re Really Getting with an Injection of Steroids
Most patients are familiar with steroid injections, but most have no idea that PRP injections are an alternative to treat many of the same issues.
Let’s review what you’re really getting when you get a steroid injection.
Cartilage Damage
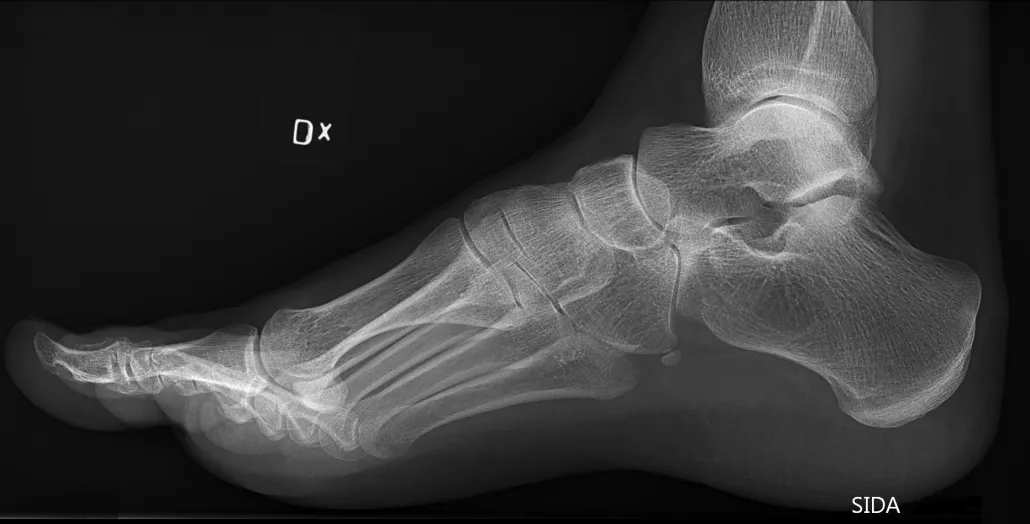
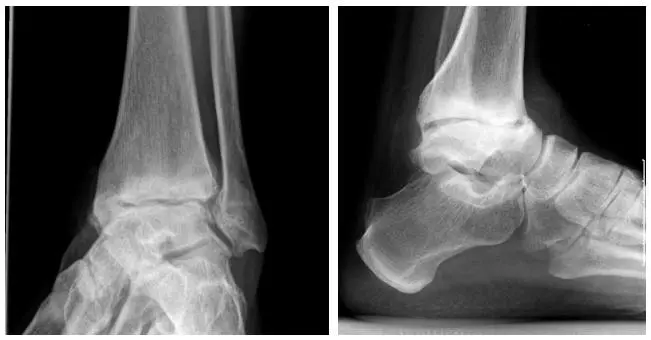
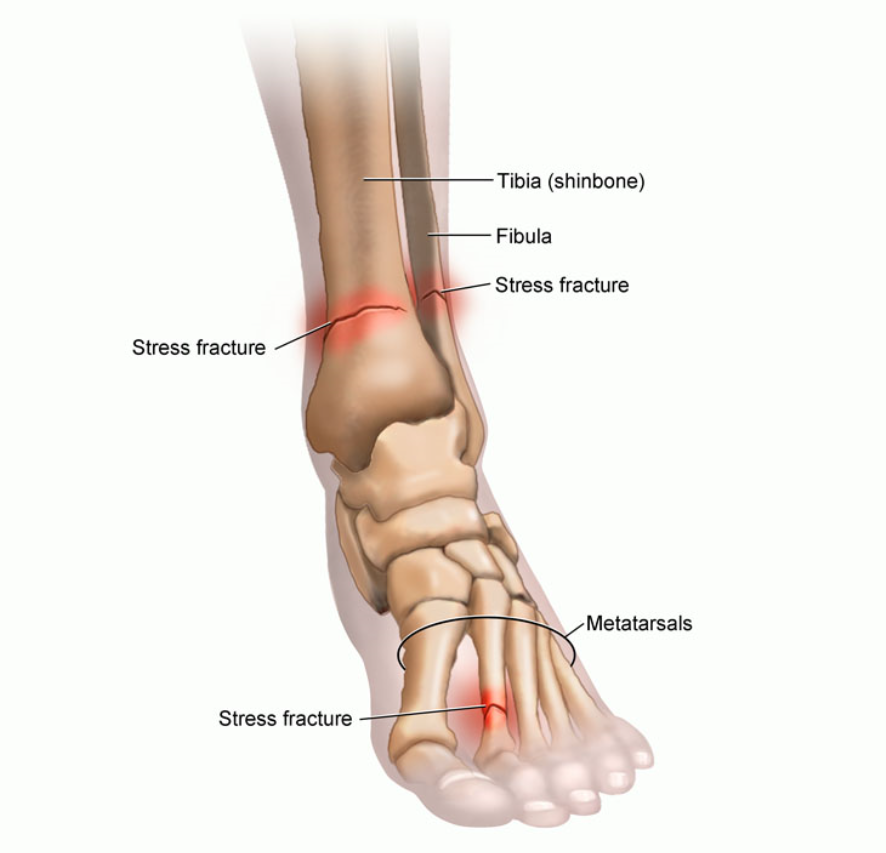
High-dose steroid injections destroy cartilage. That steroid injection into your knee, for example, might provide you with some temporary pain relief, but behind the scenes it’s wreaking havoc on your joint-cushioning cartilage. If you think you’re off the hook because your steroid injections are being injected into your foot for plantar fasciitis, think again. Your foot contains many tiny joints, all cushioned with cartilage to help provide smooth movement.
Diminishing Relief
Repeated steroid injections have been shown to provide diminishing relief with each subsequent injection. Why? Possibly because of the toxic effect steroids have on the local repairing stem cells…
Poisoned Stem Cells
Your body’s own stem cells are powerful cells that respond to damage and immediately get to work repairing it when it occurs. One study found that when mesenchymal stem cells are exposed to steroids, this, in effect, poisons the cells, stifling their ability to become bone and to repair bone. With no strong stem cells to stop it, wear and tear sets in and bone damage occurs.
Increased Risk for Bone Loss
Bone loss and osteonecrosis are well-known potential risks of steroid treatments.
Decreased Blood Supply
In order to stay healthy and effectively heal, tissues need a good blood supply. One study, however, found that when comparing patients who were undergoing rotator cuff surgery and had steroid injections prior to the surgery to those who didn’t have steroids, the steroid patients had one-third fewer blood-supply vessels.
So if you have plantar fasciitis, is there an alternative for steroid injections? Yes! Platelet rich plasma, or PRP…
What You’re Getting with an Injection of PRP
Platelet rich plasma (PRP) is concentrated from blood platelets, which are the body’s natural growth factors and healing molecules. When you have an open wound, such as a finger laceration or a skinned knee for example, it’s your platelets that rush in and start clotting your blood to stop the bleed. Your growth factors also kick in to encourage healing. It’s how the body heals itself when minor injuries occur.
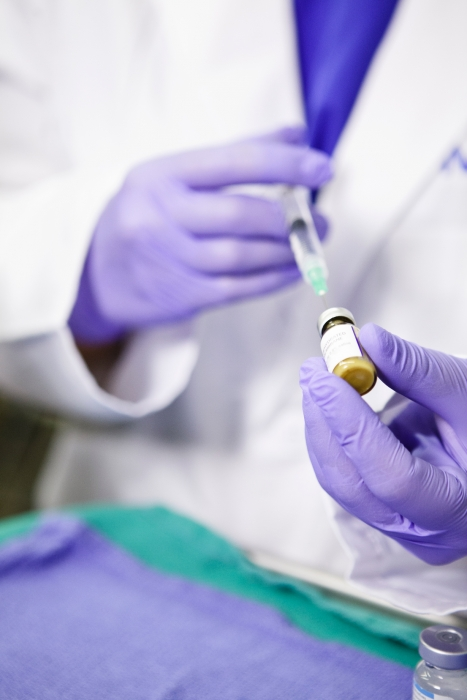
To obtain PRP, blood is drawn from a vein and the whole blood is centrifuged, or rapidly spun. Centrifuging separates the plasma serum where the platelets are concentrated; hence, the result is a platelet rich plasma.
Injections of a patient’s own PRP stimulate the body’s local stem cells to wake up and start repairing damaged tissues. So PRP is like a shot of espresso for our repairman cells. PRP is used to treat many orthopedic conditions, such as muscle, ligament, and tendon tears, sprains, arthritis, and much more.
Study Favors PRP vs Steroids for Plantar Fasciitis
The purpose of the new study (http://www.footanklesurgery-journal.com/article/S1268-7731(18)30023-7/fulltext?rss=yes) was to compare the impact of PRP versus steroid injections on chronic plantar fasciitis. Both outcomes and imaging (ultrasound and MRI) were analyzed in 40 patients with plantar fasciitis—20 received PRP and 20 received steroids. Subjects were evaluated at three and six months following treatment.
The results? While there were improvements in both groups, the PRP group showed significant improvement over the steroid group. Researchers concluded that PRP injections are a “more effective therapeutic method” than steroid injections. In addition, the study goes on to say that not only is PRP safe, but that PRP treatment provides a longer-lasting solution than steroids.
The upshot? This is one of many studies that now show that PRP is better than steroids and doesn’t have the nasty side effects. If you’re a patient who is getting or about to get a steroid injection, spend a little on yourself and upgrade to a PRP shot. You’ll be glad you did!